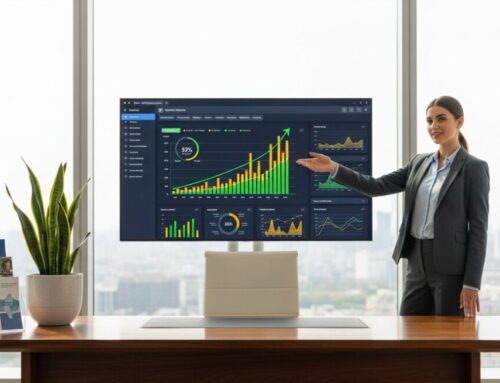
For Medicare insurance agents and agencies, the moment a transferred call connects is where revenue is won or lost. This critical handoff, where a warm lead becomes a live conversation, represents a significant investment and an even greater opportunity. Yet, many organizations treat call transfer lead performance as a black box, focusing solely on the volume of calls received rather than the quality of the engagement and the subsequent conversion. Truly understanding and optimizing this performance is the key to transforming your Medicare lead generation strategy from a cost center into a predictable growth engine. It is about moving beyond simple call counts to analyze the behaviors, signals, and outcomes that define a profitable transfer.
The Core Metrics That Define Call Transfer Success
To manage performance, you must first measure it accurately. Generic metrics like “calls per day” are insufficient. You need a dashboard built around the specific lifecycle of a transferred Medicare lead. This begins with connection rate, the percentage of transferred calls where the agent actually makes contact with the prospective client. A low connection rate often indicates issues with lead source quality, inaccurate contact information, or poorly timed transfers. The next vital metric is the qualified conversation rate. Not every connected call is a good fit. This measures the percentage of contacts that meet your basic criteria for a Medicare prospect, such as being in your service area, within the enrollment window, and genuinely interested in reviewing plans.
However, the most telling metrics occur after qualification. Engagement duration is a powerful qualitative indicator. A two-minute call is vastly different from a twenty-minute consultation. Longer talk times typically correlate with higher levels of prospect interest and agent effectiveness. Ultimately, every metric should ladder up to the appointment set rate and the final conversion rate to sale. Tracking the journey from transfer to appointment to closed policy reveals the true efficiency and ROI of your lead source. Without this closed-loop analysis, you are only seeing a fraction of the picture. For a deeper dive into the foundational difference between raw calls and actionable leads, our resource on Medicare calls vs. Medicare leads provides essential context.
Optimizing The Transfer Process For Higher Conversion
Superior performance is engineered, not accidental. The transfer process itself must be meticulously designed to preserve lead warmth and intent. First, ensure the data accompanying the transfer is rich and immediate. The agent receiving the call should have access to the lead’s name, location, the specific ad or keyword they responded to, and any pre-qualification information collected. This eliminates repetitive questions and allows the agent to personalize the conversation from the first hello. Second, speed is non-negotiable. Transfers must be instantaneous or followed up with an immediate outbound call by the agent. Every minute of delay increases the likelihood of the prospect disengaging.
The scripting and training for the initial call recipient, often a call center or automated system, are equally important. This entity must set proper expectations, clearly stating that a licensed Medicare specialist will join the call or call them back shortly. Furthermore, a smooth handoff requires robust technology. Your CRM and phone system must be integrated so that the agent’s screen pops with the lead’s information the moment the call comes through. Investing in this infrastructure eliminates friction and demonstrates professionalism. Consider these key elements for an optimized transfer protocol:
- Pre-Transfer Qualification: Capture essential data like zip code, age, and current coverage (if any) before the agent connects.
- Seamless Technology Integration: Use a CRM with screen pop functionality that auto-populates lead data on answer.
- Agent Readiness & Training: Ensure agents are trained on the lead source and have a clear script for greeting transferred calls.
- Contingency Plans: Have a clear process for missed connections, including immediate call-back protocols and follow-up email/SMS templates.
Even with a perfect process, some transfers will not connect. It is critical to have a structured follow-up campaign for these missed opportunities. An automated yet personalized sequence of emails and SMS messages can recapture a significant percentage of leads who were initially unreachable. This transforms a failed transfer into a nurtured lead.
Analyzing Lead Sources And Agent Performance Together
Medicare call transfer lead performance cannot be evaluated in a vacuum. It exists at the intersection of lead source quality and agent skill. A common mistake is to blame low conversion rates solely on agents when the underlying issue may be poor lead quality. Disaggregate your performance data by lead source. You may find that transfers from a particular digital marketing campaign have a 60% connection rate and a 25% appointment set rate, while transfers from a different partner have a 40% connection rate and a 10% appointment rate. This analysis allows you to allocate your budget toward the highest-performing sources and either improve or eliminate underperforming ones.
Concurrently, you must analyze individual agent performance within the context of the leads they receive. Look for patterns. Does one agent consistently have longer engagement durations and higher conversion rates from the same lead source as their peers? This suggests superior technique that can be identified and trained across the team. Conversely, if an agent underperforms across all lead sources, it indicates a need for coaching on call handling, product knowledge, or closing techniques. Creating a culture of data-driven coaching, where feedback is based on specific metrics like qualification rate or offer-to-appointment ratio, is far more effective than generic sales advice. Understanding what happens when Medicare call transfers fail is a crucial part of this diagnostic process, helping to close feedback loops.
Compliance: The Non-Negotiable Foundation Of Performance
In the Medicare space, high performance is meaningless without strict adherence to compliance regulations. The Centers for Medicare & Medicaid Services (CMS) have clear rules governing marketing and communications with beneficiaries. Every call transfer and subsequent conversation must be recorded and stored appropriately. Prior to discussing specific plan details, agents must obtain the beneficiary’s expressed consent, documented through a Scope of Appointment (SOA) form. The transfer process itself must be transparent; prospects cannot be transferred under false pretenses, such as being told they are calling for a free gift only to be connected to a sales agent.
Performance metrics should include compliance checkpoints. Monitor 100% of calls for required disclosures and proper consent capture. A single compliance violation can result in severe penalties, including fines and the loss of your ability to sell Medicare plans. Therefore, your training, scripting, and quality assurance programs must be built with compliance as the core, not an afterthought. This protects your business and builds trust with clients, which is ultimately a key driver of long-term performance and referrals.
Leveraging Technology For Smarter Transfers And Insights
Modern technology is the force multiplier for Medicare call transfer lead performance. Beyond basic CRM integration, consider platforms that offer predictive analytics. These systems can score leads in real-time based on the data collected pre-transfer, allowing for prioritization. A high-intent lead who clicked on a “Medicare Supplement Plan G” ad and provided their email and phone number might be routed to your top-performing agent immediately, while a lead with less data might enter a different queue. Call tracking software with dynamic number pooling can provide unparalleled source attribution, showing you not just which campaign generated a call, but which specific ad creative or keyword led to the transfer.
Furthermore, AI-powered conversation analytics tools can transcribe and analyze every transferred call. They can flag moments where agents missed an opportunity to ask for an appointment, failed to address a key objection, or deviated from compliance scripts. This provides objective, scalable data for coaching and process improvement. The goal is to create a tech stack that provides end-to-end visibility and intelligent automation, from the moment a lead clicks an ad to the final policy enrollment.
Frequently Asked Questions On Medicare Call Transfers
What is a good connection rate for transferred Medicare leads?
A strong connection rate typically falls between 50% and 70%. Rates significantly lower than this suggest potential issues with lead data accuracy, transfer timing, or the initial lead source quality. It is the first critical metric to diagnose.
How quickly should an agent call back a missed transfer?
Immediately. The best practice is to have the agent attempt the call back within 60 seconds. If no answer, a structured follow-up sequence with an SMS and email should be triggered within 5 minutes. Speed is essential to capitalize on the prospect’s intent.
Should we use a third-party call center for transfers or handle them in-house?
This depends on scale and control. In-house handling offers greater control over agent training and compliance but requires infrastructure. Third-party centers can provide scale and 24/7 coverage but require rigorous vetting, training, and monitoring to ensure quality and compliance. Many successful agencies use a hybrid model.
How do we track ROI from call transfers accurately?
You must track the full funnel. Attribute each closed policy back to the original lead source and transfer instance. Calculate your cost per lead (CPL) from the source, then your cost per acquisition (CPA) including agent time. True ROI is (lifetime value of the client) minus (CPA). This requires tight integration between your marketing, CRM, and sales data. For a comprehensive look at managing the entire lead lifecycle, including post-transfer follow-up, explore our insights on next steps after failed Medicare call transfers.
Mastering Medicare call transfer lead performance is a continuous cycle of measurement, analysis, and refinement. By focusing on the right metrics, engineering a seamless transfer process, enforcing compliance, and leveraging technology, you can systematically increase conversion rates and maximize the return on your lead generation investment. The outcome is a more efficient sales operation, higher agent morale, and sustainable business growth in the competitive Medicare marketplace.